In the bustling realm of healthcare, where the primary goal is to heal, the unfortunate reality is that hospitals sometimes become breeding grounds for infections. Hospital-acquired infections (HAIs), also known as nosocomial infections, pose a significant challenge to both patients and healthcare providers. This article delves into the world of HAIs, exploring examples, and, more importantly, the preventive measures that can be taken to mitigate these risks of clinical negligence.
Understanding Hospital Acquired Infections
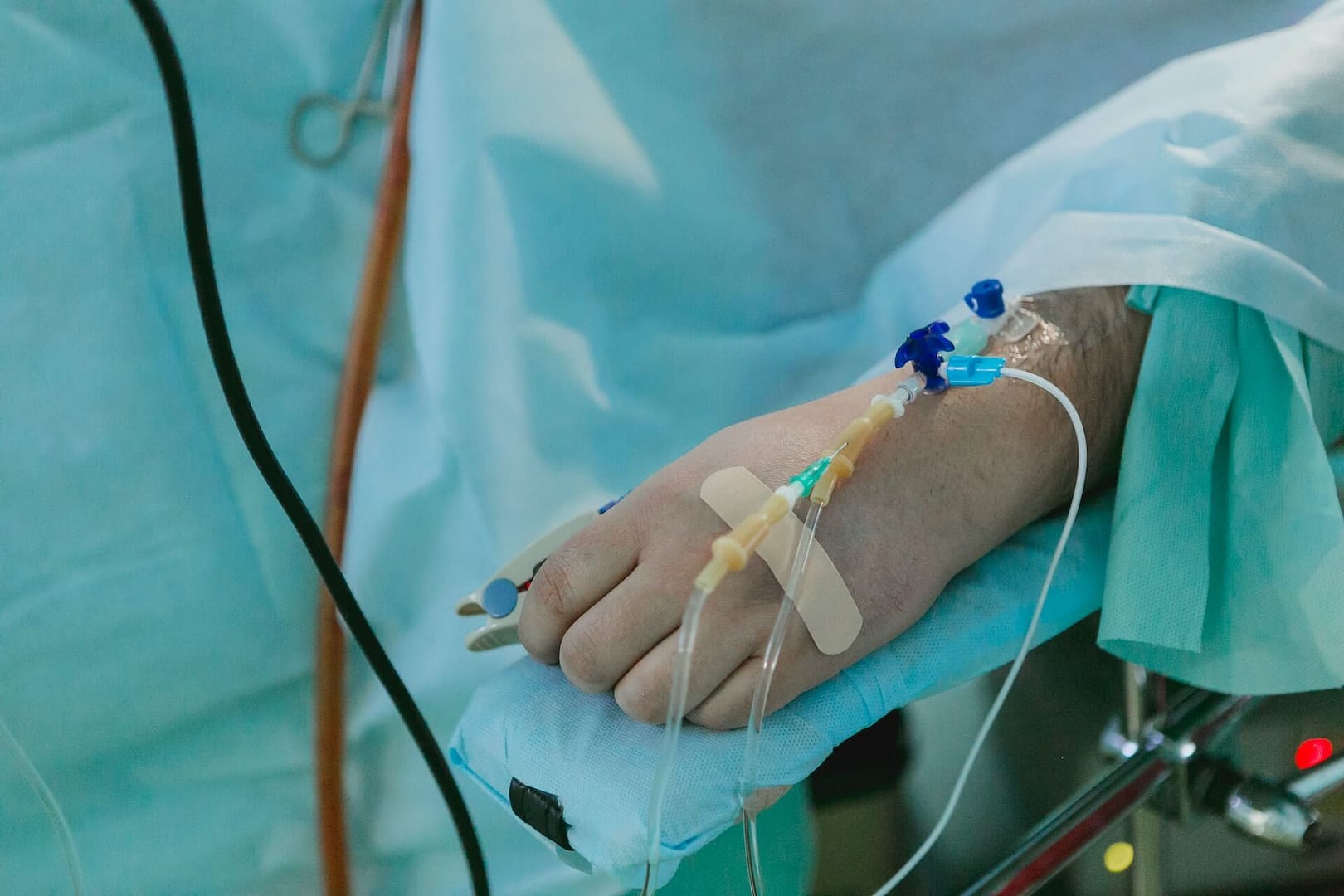
Hospital acquired infections are infections that patients acquire during the course of their hospital stay. Contrary to the expectation that hospitals are sanctuaries of health, they can inadvertently become sources of infections due to various factors. These infections can be bacterial, viral, or fungal, and they often manifest after 48 hours of hospitalisation.
One common example of a hospital-acquired infection is surgical site infections (SSIs). Imagine a scenario where a patient undergoes surgery with high hopes of a swift recovery. However, due to inadequate sterilisation procedures or negligence, the surgical wound becomes a gateway for harmful pathogens, leading to an infection that complicates the recovery process.
Examples of Hospital Acquired Infections
Let’s explore a few examples to shed light on the diverse nature of HAIs. Urinary tract infections (UTIs), often caused by catheterization, are prevalent in hospital settings. A patient admitted for an unrelated condition might end up with a secondary complication due to an oversight in catheter care. Similarly, ventilator-associated pneumonia (VAP) is another common HAI. Patients relying on ventilators are vulnerable to respiratory infections if proper protocols, such as regular tube maintenance and oral hygiene, are not strictly adhered to.
In the context of the UK healthcare system, the National Health Service (NHS) has identified several other examples, including bloodstream infections, Clostridium difficile infections, and Methicillin-resistant Staphylococcus aureus (MRSA) infections. Each case is a stark reminder of the need for rigorous infection control measures.
The Importance of Preventive Measures
Prevention is undeniably the cornerstone of addressing hospital-acquired infections. The repercussions of these infections extend beyond the physical discomfort experienced by patients; they often lead to prolonged hospital stays, increased healthcare costs, and, in severe cases, can be life-threatening. Therefore, it becomes imperative for healthcare professionals to adopt stringent preventive measures.
Hand Hygiene: The First Line of Defense
One of the most straightforward yet effective preventive measures is proper hand hygiene. It might seem like common sense, but the significance cannot be overstated. Regular handwashing, use of hand sanitisers, and adherence to hygiene protocols can significantly reduce the transmission of pathogens. The simple act of washing hands can be a powerful barrier against a multitude of infections.
Aseptic Techniques in Medical Procedures
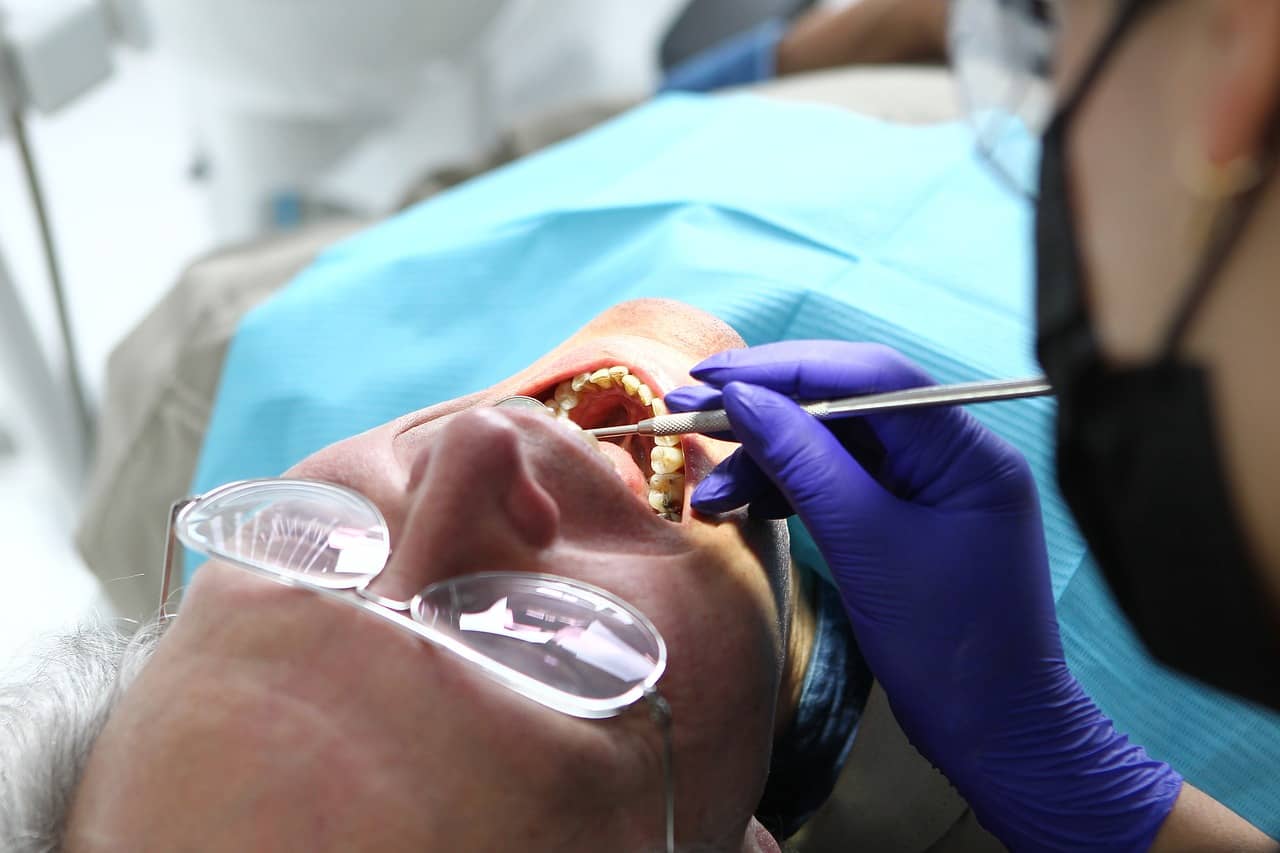
Ensuring the aseptic technique during medical procedures is paramount. From surgeries to simple injections, every invasive procedure carries the risk of introducing pathogens into the patient’s body. Strict adherence to sterile protocols, including the use of sterile gloves and equipment, minimise this risk substantially.
Environmental Hygiene: Beyond the Patient
The hospital environment itself plays a crucial role in infection prevention. Regular cleaning and disinfection of surfaces, equipment, and shared spaces can curb the spread of pathogens. The emphasis should not only be on patient rooms but also on commonly used areas such as waiting rooms and corridors. A clean environment contributes significantly to the overall safety of patients.
Education and Training for Healthcare Staff
An often overlooked but vital aspect of infection prevention is the continuous education and training of healthcare staff. Keeping medical professionals updated on the latest infection control guidelines, best practices, and emerging threats equips them with the knowledge to implement effective preventive measures. In a dynamic healthcare landscape, education is the key to staying ahead of evolving challenges.
Patient Empowerment: An Active Role in Prevention
Patients themselves can play an active role in infection prevention. Empowering patients with knowledge about the importance of hygiene, the signs of infection, and the necessity of reporting symptoms promptly can create a collaborative approach to healthcare. When patients become partners in their own well-being, the collective effort to prevent infections gains momentum.
The UK Perspective on Preventive Measures
In the United Kingdom, where the National Health Service (NHS) is at the forefront of healthcare delivery, there is a concerted effort to implement and enforce preventive measures against hospital-acquired infections. The NHS provides guidelines, protocols, and training for healthcare professionals to ensure a standardised and rigorous approach to infection control.
NHS Hand Hygiene Campaigns
The NHS has been proactive in promoting hand hygiene campaigns to raise awareness among healthcare workers, patients, and visitors. These campaigns emphasise the significance of handwashing in reducing the spread of infections. By making hand hygiene a collective responsibility, the NHS aims to create a culture where infection prevention becomes second nature.
Robust Surveillance Systems
Surveillance is a critical component of infection control, and the NHS employs robust surveillance systems to monitor and track the incidence of hospital-acquired infections. This data-driven approach allows healthcare providers to identify trends, implement targeted interventions, and continuously improve infection prevention strategies.
Collaborative Efforts Across Disciplines
In the UK, the battle against hospital-acquired infections is a collaborative effort that spans various disciplines within healthcare. Multidisciplinary teams work together to develop and implement infection control policies. This collaborative approach ensures that preventive measures are comprehensive, addressing every possible avenue of infection transmission.
Making a Clinical Negligence Claim with National Claims
In unfortunate instances where preventive measures fall short, and patients suffer due to clinical negligence, it is crucial to know the avenues for seeking justice. National Claims understands the claims process and provides a supportive framework for individuals seeking compensation. If you believe you or a loved one has suffered due to negligence in a healthcare setting, National Claims is here to guide you through the process of making a claim.

Conclusion
In the complex landscape of healthcare, where the mission is to heal, the threat of hospital-acquired infections looms. However, through stringent preventive measures and a collaborative approach, the healthcare community, particularly in the UK, is actively working to turn the tide. From hand hygiene campaigns to aseptic techniques and environmental cleanliness, every measure contributes to a safer healthcare environment. As patients and healthcare providers join forces in the battle against infections, the narrative shifts from the challenges posed by HAIs to the victories achieved through proactive prevention. National Claims stands as a beacon for those affected by clinical negligence, offering a path towards accountability and redress.
Contact us today to get a start on your claim and speak to one of our claims specialists to give you further guidance.
Click below to see why we are one of the most trusted claims management companies in the UK.

We’re proud of our excellent customer reviews
We thrive on delivering exceptional service and ensuring our clients’ satisfaction. Don’t just take our word for it. Check out some of our independent reviews to see what our clients have to say.
Excellent

This firm is excellent, they sorted out my car pay out and injury claim very fast, they always communicate with you all the time.

My accident case was dealt with confidence and with great result of the outcome, especially James kept me informed all the time.

I was very impressed at the way my inquiry was treated. I was listened to attentively and everything I needed to know was explained to me.